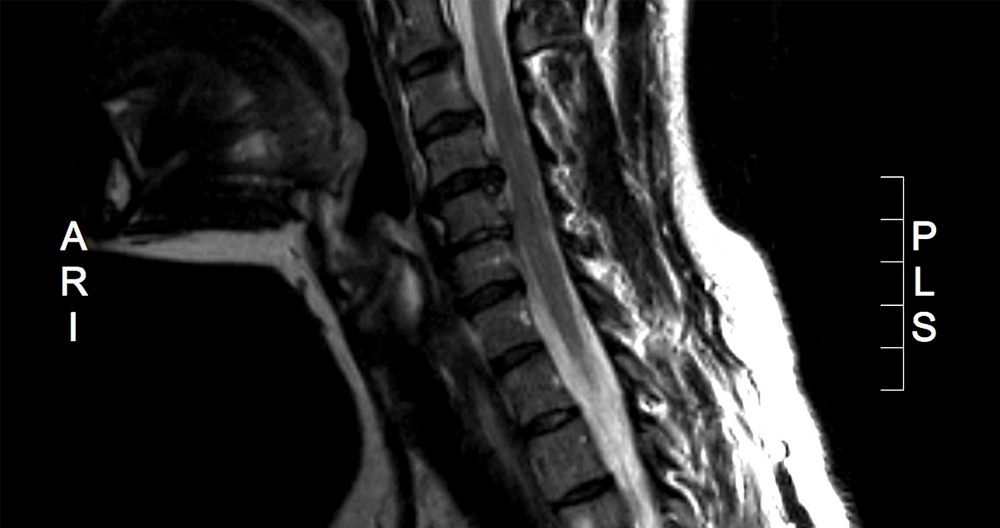
Magnetic Resonance Imaging, also known as MRI, is one of modern medicine’s most important inventions. The MRI allows surgeons to accurately diagnose and treat conditions that could potentially lead to life-threatening complications. MRIs can be useful in many areas of medicine, but they are especially helpful in the investigation of conditions in the spine. MRI scans of herniated discs can be a useful test to pinpoint the exact location and extent of the problem. Patients complaining of symptoms due to herniated discs should get an MRI scan performed first.
MRI scans are the most non-invasive way to detect bulging and herniated discs. With an MRI scan doctors can pinpoint herniated discs in their spine with over 95% accuracy due to the high spatial resolution of the spinal anatomy.
CT scans are not safe and can be inaccurate due to factors that decrease the visibility of soft tissue structural changes caused by a herniated disc. CT scans are the best way to examine spinal alignment and bony problems such as spine fractures. MRI scans can provide a detailed representation of the spinal discs as well as any problems that may be occurring around them, such degeneration or inflammation. MRI is the best method to evaluate disc injuries.
What is a Herniated Disc MRI? And When Might You Need One
MRI scans can be used to diagnose and monitor herniated discs. They are most commonly used to determine the location of herniated discs in the spine and determine the extent of nerve compression. Your doctor may recommend additional tests if the MRI results show a herniated disc. MRIs can be used to diagnose bulging discs or herniated discs in the neck or back.
What your doctor might do
The technician performing your MRI will place your body in a tube-like device after your doctor has ordered it. The magnet rotates around the patient’s body to change the excitation level of hydrogen atoms in tissues. After the magnetic field has been removed, hydrogen atoms will return to their normal resonance state. The scanner may detect this energy to create the image known as an MRI scan.
An MRI scan image generated by the scanner shows anatomy. It distinguishes between tissues that have a lot of water (such cerebrospinal fluid, discs, or other fluids) and those with less water (such skin, bone, cartilage and nerve roots). Your doctor will inspect the image for any abnormalities to diagnose your condition. MRI scans can detect disc injuries like a bulging disc, bulging disc, or annular tear that causes back pain or pinched nerve.
MRI protocol
It is very easy to use MRI for the examination of the lumbar spine of patients suffering from nerve compression symptoms. We rely on the T1W and T2W images of the sagittal and correlate them with the T2W images of the suspected levels. You should not use a saturation line on the anterior or rectangular field of vision (RFOV) because you want to image prevertebral soft tissue.
Low back pain can also be caused by an aneurysm in the abdominal aorta. Sometimes, it is difficult to distinguish neurogenic claudication (which is caused by spinal stenosis) from vascular claudication (which is caused by arterial stenosis). The frequency-encoding should take place in the AP direction and, consequently, the phase-encoding feet head.
There are many benefits to this:
- The frequency-encoded direction has the best resolution.
- To find small herniations or delineation nerve roots, we need the best resolution in the AP direction.
- Breathing artifacts are created when the phase encoding is in the AP direction. This is why some people use the RFOV or a saturation band.
- These problems are eliminated with frequency-encoding in AP-direction. You don’t even need a saturation band.
- Frequency encoding can cause poor delineation in the feet-head direction due to a chemical shift artifact, which occurs when the fat in a vertebral body meets water in a disc.
- Another reason to use an AP frequency encoder and a feet-head phase encryption is this.
It is preferable to keep the slices parallel to the nerve compression level. This method has the advantage of allowing you to follow the affected nerve through the four levels of possible compression. If you look at multiple levels of angulation, such as the one shown on the right above, you won’t be able to follow all the nerve tracts. You will also not see the whole picture.
How to read an MRI of a Herniated Disc
There are many factors that affect the interpretation of an MRI scanner. Similar to other diagnostic tests, the problem with MRI scans is that the “disorder”, as it appears on the MRI scan, may not be the source of backaches.
A lumbar MRI scan of a herniated disc will be accurate if the patient has a basic understanding about the anatomy of the lumbar spine. There are five components to the lower back. They are separated by two types of joint, facet and discs. These discs are often in constant motion, which causes wear and tear. An annular tear is when the outer disc layer ruptures and the inner nucleus jelly of the disc pushes into the spinal canal, forming a hernia. An MRI scan will often reveal this hernia as a contrast spot.
The patient’s physiological symptoms and experiences will guide MRI scan results. A herniated disc may not cause symptoms, so there are many people who have undiagnosed back conditions. If the herniated disc becomes protruding or bulging, it can cause severe pains.
The most common cause of back pain is when the herniated disc becomes inflamed along a posterior annular tear. This causes pain signals to travel via a sinu-vertebral neural located along the margin -in of the annulus fibrosus. The nerve fibers running along the annulus fibrosus posterior wall are somatic pain fibers (SA) and will project their pain signals into a part of the brain that is responsible for highly localized pain, the primary somatosensory cortex.
Evaluation of MRI Scan Results
The first problem with MRI scans, like many other diagnostic studies, is that the “abnormality”, which shows up on the MRI scan, may not be the reason for back pain. Many clinical studies have found that around 30% of people in their thirties or forties show a lumbar disc herniation on an MRI scan. However, they don’t have back pain.
An MRI scan can’t be interpreted by itself. Every detail on an MRI scan must be correlated with the patient’s individual situation.
- The symptoms (such as the severity, duration, and location of pain)
- Any neurological deficiencies that are detected during a physical examination
The timing of the scan is also important when MRI scans are being done. An MRI scan will not be required if a patient is experiencing any of the following:
- Incontinence in the bladder or bowel
- Nerve damage can cause progressive weakness in the legs.
How to get an MRI scan to diagnose back problems
MRI scans are recommended for patients with leg pain that is not due to a lumbar disc herniation. Because surgery to repair a lumbar disc herniation usually has few side effects (morbidity), and allows for an early return of normal function.
Patients suffering from primarily lower back pain should consider lumbar spine fusion. This type of spine surgery can have some side effects (morbidity) that may be more severe than expected and take longer to heal. Doctors recommend that patients wait 3 to 6 months after the onset of low-back pain before getting an MRI scan to determine if conservative (nonsurgical)treatments will be able to alleviate the pain.
In most cases, if the results from the MRI scan do not affect a patient’s future back pain treatment, and the patient continues with non-surgical treatments like chiropractic treatments and physical therapy, then waiting to have an MRI scan is a reasonable option.