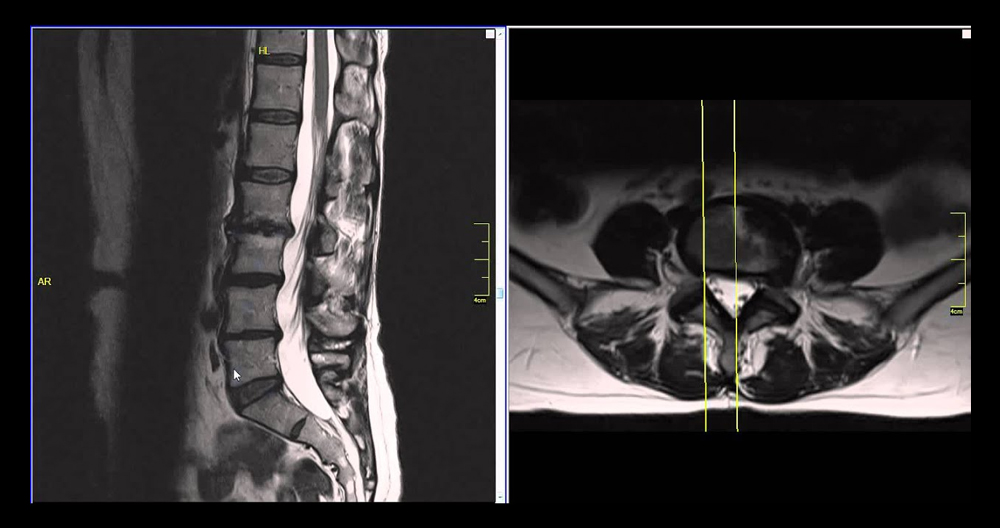
Slipped Disc? An MRI is a must to detect a herniated disc
A herniated disc (also known as a slipped or ruptured disc) is a condition that occurs when a disc ruptures due to old age, degeneration, or an injury or accident. This causes a small amount of the soft cartilage to be pushed out from the outer, hard shell. Although herniated disks may not cause symptoms, sometimes severe pain can result. For example, Herniated sciatica is when the disc herniation is located in the lower back. This presses on the sciatic nerve. While most people will find that a slipped disk heals on its own, some cases may require therapy or surgery.
What are the Signs and Symptoms for a Ruptured Disc
The spine is made up of complex bony structures. Each vertebrae are protected by a disc-shaped structure that protects them from injury and cushions them from any impact.
The outer layer of each disc is called the annulus. It consists of a soft inner cartilage called nucleus pulposus. The nucleus pulposus pushes outwards when the annulus becomes brittle due to injury, overuse or aging.
This can lead to nerve damage and pressure that is greater than normal. This causes a painful sensation and can lead to permanent nerve or spine damage.
The symptoms of a ruptured disk can vary from one person to the next. It is important to determine the exact location and size of the herniated disk. The severity of the following symptoms and signs can also depend on how healthy an individual is.
- Lower back pain
- Radiating pain from the back to the extremities
- Difficulty in movement
- Numbness on one side or the other of the body.
- Extreme and unusual muscle weakness
- Frequent tingling or pain in the affected area
How can a herniated disc be diagnosed?
The consulting Healthcare Professional won’t always recommend an MRI if a patient presents with any of the above symptoms or signs during a physical exam. Usually, an MRI is not necessary unless chronic pain persists for more than 6 weeks after using conservative treatments such as massages and stretching exercises.
Patients with herniated discs of the neck or lower back are most likely to recover after non-surgical treatment. Others may need a more detailed examination or diagnostic imaging in order to confirm.
Imaging tests are used to confirm the existence of a herniated disk, especially when surgery is required. A CT scan, MRI scan or x-ray may be required to confirm the presence of a herniated disc in the neck or other area of the spine where pain is reported.
MRI is the best imaging procedure available to diagnose a herniated disk. A MRI scan can pinpoint the location of the herniated disc and allow for the measurement of herniation.
An MRI scan can help to improve the accuracy of surgery and speed up the recovery process.
Any unusual pain in the spine should be referred to a doctor. Early diagnosis and treatment of a bulging disc or ruptured disc is possible. If the condition is not treated quickly, it can lead to irreversible complications.
Discussion
Although MRI can be helpful in certain clinical situations of lumbar back pain, it is not sufficient to assess the entire patient. Understanding the limitations and benefits of MRI when evaluating lumbar pain should help in the management of radiologically matched clinical issues.
There are many modalities for spinal imaging. Primary care physicians are now exposed to the nomenclature used by neuroradiologists as well as specialists in the field. This article will clarify commonly used terms and their clinical implications in lumbar spine imaging.
Clinical presentation
Many patients with spinal pathology present with multiple symptoms. It is important to distinguish the most common symptoms, namely lumbar back pain and sciatica. This can help in diagnosing the cause of the symptoms. Magnetic resonance imaging (MRI), while sensitive in detecting spinal pathology, is often able to detect a variety of conditions that may not have any clinical significance.
Lumbar back pain could be caused by a variety of conditions, including muscular strain and facet joint arthritis. As the name suggests, the pain is mostly localized in the back and usually arises from locally affected structures.
Sciatica is a condition that causes irritation of the nerve root and has a different distribution pattern. This may be caused by the compression of intervertebral disk herniation on nerve roots or an underlying inflammation process such as infection that causes acute pain in the distribution of a dermatome.
According to the cause of the claudication, it can be divided into either neurogenic or vasogenic categories. It can cause impaired mobility and dull, aching pain in the lower extremities. Neurogenic claudication is common in the central vertebral canal. It is variable and causes a variety of symptoms. Vascular claudication is more consistent and predictable.
It is crucial to determine symptom chronicity, identify red flags in the history, and perform a clinical examination. These are critical in determining the clinical diagnosis. They also help distinguish benign causes (e.g. musculoskeletal strain) from more serious conditions like epidural abscesses and spinal metastases. Some risk factors, such as age and medication history (eg. Ankylosing Spondylitis and compression fractures may be suspected if there is a history of steroid use or a pattern of stiffness. Further investigation would be necessary using appropriate imaging and serum tests.
Magnetic Resonance Imaging
Proton resonance technology is used to create soft tissue cross-sectional images of the spine using magnetic resonance imaging. These images allow the diagnostician more precise and detailed assessments of the intervertebral disk and its relationship to the neural structures. They are more accurate than traditional methods such as computed tomography (CT), and lumbar myelograms.
A systematic review of the available literature involving spinal MRI found MRI to be a highly sensitive and but less specific imaging modality for lumbar spinal conditions.For example, high sensitivity ranging between 89-100% for disc herniation have been described in previous studies.The lower specificity, 43-97% for disc herniation has been highlighted in previous literature and relates to the prevalence of asymptomatic disc degeneration and protrusions resulting in a large number of false positives.6 In a group of 57 patients with unilateral lower limb radiculopathy, only 30% of these patients had MRI findings of disc herniation and nerve root compression at the same level as the clinical prediction.Therefore, when reviewing the imaging, one must exert a degree of care when attributing the patient’s symptoms to the appearance of their lumbar spine.
Anatomy of the Lumbar Spine
The lumbar spine is made up of five distinct vertebrae, separated by intervertebral disks. It is reinforced by multiple ligaments as well as paravertebral muscle. The central vertebral canal contains the thecal sac, which houses the nerve roots and conus medullaris. The nerve roots exit the spine via intervertebral canal foraminal canal obliquely, instead of at right angles as is the case in cervical spine. This anatomical relationship allows clinicians to identify the nerve root that is being affected by herniated intervertebral disk.
The neural foramen is where the existing nerve roots cross. This section is divided based on the relationship it has with the pedicle or zygapophyseal joint in both the axial and the sagittal planes. The existing nerve root travels through the subarticular recess in the axial plane. It crosses the central zone and the extra-foraminal and foraminal zones. The areas along the longitudinal line are separated at the disc, supra-pedicular (pedicular), pedicular, and supra-pedicular levels.
The intervertebral discs contain a hydrated nucleus of pulposus within concentric rings made up of annulus fibrosus. As we age, our discs become more brittle, causing a decrease of T2 signal. This is often seen in patients who are asymptomatic.
Spondylolisthesis
Spondylolisthesis refers to a condition in which the lumbar spine is misaligned. This can manifest as a vertebra moving out of its normal position relative to the inferior vertebra. This could lead to narrowing of both the central spinal canal and the lateral neural foramen. Pars defects and lumbar Spondylosis are often associated with spondylolisthesis. Patients suffering from chronic pain and complex mechanical problems relating to spinal misalignment may need surgery to fuse the affected levels.
Anterolisthesis occurs at the L4-5 level. This causes severe central canal and neural fominal stenosis, as well as nerve impingement.
MRI imaging is used to assess the severity of central spinal canal stenosis and neural foramen, as well as to identify potential causes such a pars defect. Stability at the affected level can be difficult due to the static nature MRI imaging taken with the patient lying down. To assess the possibility of exaggerated spinal malalignment, spinal surgeons use dynamic lumbar spine plain X-rays. This can lead to nerve impingement and further stenosis. Future studies may include dynamic MRI spinal imaging.
Most Frequently Asked Questions
An MRI is necessary to diagnose a herniated disk
Some doctors still recommend CT scanning and X-rays. Herniated disc MRI remains the preferred diagnostic procedure for this condition. It is highly sensitive and doesn’t expose the patient to unnecessary radiation. However, MRI scanning may be delayed by clinicians if there are persistent or worsening symptoms and signs. A combination of conservative management options may be recommended to the patient in order to relieve the pain and improve their condition. Most people will be able to recover with minor surgery or other procedures. However, there are some cases that require additional investigation and treatment. This is where an MRI is often recommended.
Is a herniated disc the same thing as a ruptured disk?
The same condition, herniated disc or ruptured disc, is characterized by more protrusion than a bulging disc. A scan will show that the soft cartilage, which is normally kept inside, leaks out to the harder outer cartilage. It will also likely cause more pain than a bulging disk because it presses on nerves.
What happens if the herniated disc is not treated?
The risk of a herniated disk getting worse if it is not treated promptly increases. Slipped disc cases can be treated without the need for surgery. The non-surgical treatment of a herniated disk includes relaxation, physical therapy, and painkillers. If the condition is not treated, it can cause permanent nerve damage. People with this condition have reported losing bladder control and bowel control as well as feeling around the legs and rectum.
Can MRI be used to detect herniated discs?
An MRI scan can confirm a herniated disk diagnosis. It pinpoints the exact spot on the spine where there is herniation. It is possible to manage treatment (which may include surgery in certain cases) better and optimize patient recovery.
What causes herniated discs?
There are many reasons that a herniated disk can occur. A major cause of disc herniation is not only accidents but also normal wear and tear on the spine due to aging. The following are possible causes:
- Poor posture
- Doing heavy lifting, especially in an unsuitable position, can cause unnecessary strain to the back.
- Obesity or being overweight can cause unnecessary pressure on your spine. Weak muscles
- Inactivity and lack of regular exercise
Summary
Understanding the limitations and benefits of MRI when evaluating lumbar pain can help to improve the treatment of radiologically matched clinical issues.