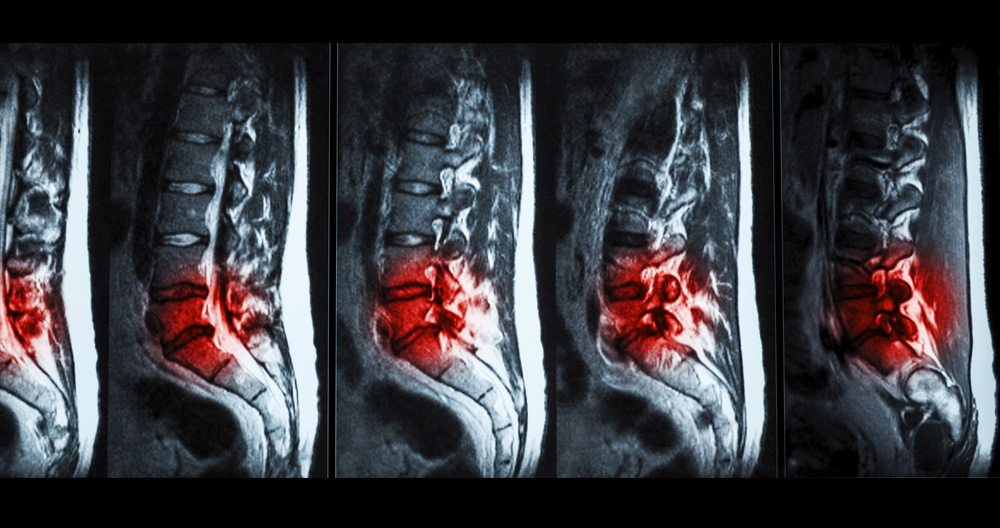
The L5–S1 spinal segment can be found just below the beltline. It is the last segment in the lower back that articulates with the sacrum (tailbone). Research has shown that at least 80% of adults will experience pain in the back at one time or another. The disorders of the three most common lumbar segments, L3-L4, l4-l5, and s1 are the main causes of back pain. Two of the most common back pain segments are L4-L5 (or L5-S1)
The Spine is divided into five sections.
- The total number of vertebrae in the cervical spine (neck), is seven.
- The twelve vertebrae that make up the thoracic (upper and middle back) spine are twelve
- The Lumbar spine, lower back, is made up of five vertebrae.
- Sacrum, triangular bone, that connects with L5, both pelvises and the coccyx, to form the tailbone. The small triangular-shaped structure of the spine at the bottom is the coccyx.
INTRODUCTION
Low back pain (LBP), which is the most common problem, is a leading cause of disability. Herniated lumbar disc is one of many abnormalities that are associated with LBP. Lumbar discectomy is a procedure that has been performed regularly by neurosurgeons for many decades. Radiculopathy and back discomfort are the most common signs. Incontinence or rectal dysfunction may occur if there is urinary retention.
Saddle anesthesia should be suspected of CES. However, it is not clear what its pathophysiological mechanisms are. It can be due to direct mechanical compression or Cauda Equina (CE), nerve roots. This is a common condition that can cause work disability. The rare occurrence of sexual and sphincter dysfunction in the CES is due to a prolapsed lumbar lumbar L5–S1 intervertebral Disc, but it has not been thoroughly investigated. This study examines the potential mechanism and outcome of the sexual dysfunction and sphincter dysfunction that can be associated with lumbar disc herniation.
Back Pain and The L5–S1 Spinal Segment
The lower lumbar spinal column is susceptible to injury and wear. A variety of conditions and diseases can impact daily life, including lumbar spine problems.
These are the symptoms and conditions associated with an L5–S1 spinal segment disorder.
- Leg pain, back pain, and pain in the buttocks are all possible.
- Numbness, tingling or burning sensations in your buttocks or legs, feet, feet, or toes
- Problems walking, or inability to stand for a short time
- Paralysis of one or both legs
- Bowel and Bladder disorders
- Sexual dysfunction, including impotence and infertility
The Best L5/S1 Treatment Option
The best way to treat spinal disorders such as L3-L4, L4–L5, L5–S1, and L5–S1 is to be conservative. It is best to avoid any invasive procedures like steroid injections, radiofrequency ablation (RFA), or spine surgery.
Radiofrequency ablation (or RF ablation) is a minimally-invasive spine surgical procedure. It kills the pain-sensing neuron in your spine. Patients should be discouraged from receiving this treatment, as it can cause degenerative changes to the spine due to nerve damage or soft tissue destabilization.
For back pain due to L3–L4, L4–L5, or L5–S1, you need targeted conservative treatments that treat the affected or injured areas. A combination of chiropractic and physiotherapy is the best treatment for back pain. Pain and disabilities are most common in the lower lumbar segments L3-S1. Slip-discs, arthritis (bone spurs), degenerative discs and arthritis are all common causes of back and leg pain.
L5-S1 Spinal Segment Issues Which Cause Back Pain & Leg Symptoms
Back pain sufferers often experience problems with the L5–S1 segment. These conditions may cause back pain that is caused by the L5–S1 segment.
- Muscle spasms (in some cases): This is the first sign of backache.
- Joint problems: Spinal joint misalignment or arthritis can cause back pain. A neglected spinal problem can lead to other serious problems like bone spurs, facet hypertrophy and slipped discs.
- Pinched nerves: A pinched nerve is the result of slipped discs, bone Spurs, and ligament thickening. This can be seen in Ligamentum Flavum facet hypertrophy or hypertrophy.
- L5 – S1 Spondylolisthesis: In L5 – S1 Spondylolisthesis, the 5th lumbar section (L5) moves forward relative to the first sacral segments (S1). L5-S1 is the most common location for spondylolisthesis. L5 to S1 is the most common location for spondylolisthesis. L5-S1 can have spondylolisthesis that is either congenital (due to a fracture, spondylolysis), or developmental.
- Degenerative changes are: Spinal disc degeneration, spinal joint degeneration, or soft tissue degeneration (degenerated muscles, ligaments, and spinal disc slipping) are all leading causes of back pain. Degeneration of your discs or soft tissue may be the cause of back pain.
- Slipped disc: The term “slipped disc” is used by laypeople to describe bulging discs and herniated discs.
- Sciatica: A collection of nerves originating from spinal nerves exiting from L4 to S3 is called the sciatic nerve. The L5-S1 section is the major nerve involved in sciatica, or sciatic-like symptoms.
- L5 to S1 spondylosis: This is a condition that causes excessive weight-bearing or repetitive injuries.
- Posterior Facet hypertrophy at L5–S1: This is the medical term for the spinal joints. Each segment contains four facets. Spinal joints are formed when the facets of the vertebrae below are connected to the above facets. Facet hypertrophy can be the primary cause of backache.
- Spinal canal Stenosis L5-S1: When the cord is gone, the spinal canal acts as a tunnel or passageway to the spinal cord. The L1 is the end of the spinal cord. It continues to descend as nerve fibers which look like horse’s tail hairs. Spondylosis and spondylolisthesis are the most common causes for spinal canal shrinkage.
- Hypertrophy and Ligamentum Flavum at S5-S1: Ligamentum Flavum connects spine bones and provides stability. This ligament is essential for extending and bending movements. Ligamentum Flavum can thin at any segment. The L5–S1 segment does not have as many cases of hypertrophy (or thinning) of Ligamentum Flavum as the L3–L4 and L4–L5 segments.
- L5-S1 foraminal Stenosis: The openings that allow nerves to exit the spine through. Nerve impingement is caused by shrinkage of the foramen. Foraminal or vertebral foraminal stenosis, also known as foraminal foraminal swelling, is common in the slip disc, spondylolisthesis (hole), facet hypertrophy and hypertrophy Ligamentum Flavum.
You need to seek expert help to heal from L5-S1. Here are some steps to help you with your back pain treatment.
Back Pain from L5-S1 Problems
Two of the most common causes of back pain are L4-L5 (L5-S1) and L5–S1 (L5-S1). The main cause of problems arising from L5–S1 is axial loading (weight-bearing actions). Sitting or standing for long periods of time places enormous stress on L5-S1 segments’ spinal joints and discs. Increased intradiscal pressure is a result of excessive or prolonged weight-bearing.
Indical pressure is measured as mm Hg (millimeters). A healthy intradiscal level is less than 70 mm Hg. An increase in intradiscal pressures above 90 mmHg can cause a decrease of blood flow. An increase in intradiscal pressure also means that nutrients and compounds are not being absorbed into the spinal disc.
The intradiscal pressure, or spine disc pressure, is directly affected by body position and daily activities. These are examples of the average intradiscal pressure at various positions:
- Supine position: The intradiscal pressure average is 25 mmHg
- Standing straight: Intradiscal pressure goes up to 100+mm Hg
- While standing, bend at the waist and let your belly rise to 150+mm Hg.
- Sitting straight up: The Average Intradiscal Pressure is 200 mmHg
- Sitting in poor positions: The intradiscal pressure can rise to 250+mm Hg
The most vulnerable spinal segment is the lumbar spine (lower back), which is subject to the adverse effects of higher intradiscal pressures that are associated with prolonged standing or sitting.
L5-S1 Disc Bulge And Disc Herniation Causes, Signs & Symptoms
The most common place for disc bulge, disc herniation (slipped disc) is in the lower back or lumbar spine. L4-L5 are the most common locations for a slipped disc to develop in the lower spine. L5-S1 is second in the list of possible involvement. L3-L4 is the most common site of herniated Lumbar discs.
Degenerative disc disease, which causes spinal disc herniation at L5 and S1, is the most common cause. Spinal disc diseases are all connected to disc degeneration. For L5-S1 to herniate, the disc must have had pre-existing degenerative conditions. Healthy discs will not herniate. Degenerated or damaged discs can lead to a herniated disc L5-S1. These are the most common causes of herniated spinal discs:
- Prolong sitting
- Sit in a forward bent position
- Excessive bending and twisting of the back
- Improper lifting
- Slip and fall
- Injuries
A herniated L5S1 disc could press and impinge nerves or the spinal cord. It can lead to pain, discomfort, and aches in the back, buttocks. It can also cause weakness, tingling and numbness in the legs, legs or knees.
L5-S1 pinched nervous symptoms include weakness, stiffness and numbness. Nerve pain refers to pain that is burning, sharp, or throbbing-like and can travel to the lower extremities, giving patients sciatica-like sensations.
Sciatica is caused by one or more nerves in your cervical spine being compressed, or irritated. You may feel a burning or shooting sensation in your lower back. The pain then moves up your leg and affects the nerve distribution in your feet. Sciatica pain may radiate to the buttocks. Its distribution is dependent on the nerves affected.
L5-S1 Spinal Segment Issues: Back Pain & Leg Symptoms
Low back pain and leg pain are common symptoms of spine problems. However, patients who have severe neck, upper back or mid-back issues and compress their spinal cords may experience weakness and pain in the legs. It is important to get expert help and analysis in order to determine the exact cause of leg discomfort.
If a slipped disc (disc bulge, herniated disc), presses on a nerve, it can cause pain, weakness, or numbness in the area where the nerve travels. The cause of pain felt in the legs and buttocks could be from compression of nerves, an L4–L5 or L5–S1 impingement on spinal nerves, or the compression of the thecal sac.
A bulging or herniated spinal disc can happen at any part of the spine. The neck and lower back are known for bulging, herniated and slipped discs. Slipped discs may occur in the neck at the C4-C5, or C5-C6 segment. Slipped discs are most common in the lower back at the L3–L4, L4–L5, or the L5–S1.
Sciatica-like sensations are common symptoms of back pain caused by herniated discs or slipped discs. They include pain and numbness around the buttocks, leg, foot, toes, and thigh. It can also lead to pain and numbness in your genital area, difficulty with urinating, weakness in the legs, and even a loss of sensation.
Sciatica & The Sciatica-S1 Spinal Segment
Sciatica refers to pain in the back and hips that results from compression of the sciatica nerve, which runs from the lower part of the spine to the lower extremities.
Sciatica is a condition where nerve fibers from sciatica are compressed in the spine, thecal sac or exiting to the spine. Sciatica may also be caused due to congenital abnormalities or excessive muscle tightness. This is a deep muscle found in the buttocks.
Spinal Canal Stenosis – Common Causes of Back Pain
The spinal canal is a tunnel made by the interlocking spine segments that house the spinal cord. The spinal cord is an elongated, cylinder-shaped bundle made up of nerves. It begins at the skull’s base. It then descends into the spinal canal until it reaches the L1 segment or the first lumbar.
The L1-L2 level of the spinal cord is when the spinal cord becomes a solid rope-like cylindrical to strands like a horse’s tail. (solid part and hair strands). The point at which the rope-like structures transform into hair-like roots or strands is known as cauda Equa.
Cauda Equina Syndrome & Back Pain
Cauda Equina Syndrome is caused by compression and impingement in the nerves in the lower spine (nerves of the spinal canal). Cauda Equina syndrome is most commonly caused by slipped disc, arthritis, hypertrophy and Ligamentum Flavum. These causes compress the spinal cord, spinal sac and nerve roots as they exit from the spinal canal. Cauda Equina Syndrome is a mix of all three.
Cauda equina Syndrome is associated with severe pain in the lower back and lower extremities. This syndrome can lead to paraesthesia, weakness, difficulty in walking and even intestinal and bladder problems in severe cases.
Cauda Equina syndrome symptoms include severe pain in the lower back and legs, paraesthesia, weakness, and difficulty walking in the feet. Cauda equina can also present with other symptoms, such as sexual and reproductive problems, bowel or intestinal issues, bladder disorders, and bladder disorders.
Cauda Equina Syndrome can be caused by most common spinal segments, L4-L5 (S1 and L5-S1). These conditions include slipped discs and thickening of posterior vertebral bodies (spondylosis/arthritis and bone spurs) and hypertrophy at the Ligamentum Flavum.
Anatomy of L5-S1 Spinal Motion Segment
The following structures are typical of this motion segment:
L5 and S1 vertebrae. Different features distinguish the L5 from S1 vertebrae.
- L5 includes a vertebral body at the front and an arch at back. The arch has 3 bony protrusions. There is a prominent spinous center and two transverse processes on each side. These protrusions act as attachment points to ligaments.
- The sacral base (also known as S1) is the top and wider end of the triangularly-shaped sacrum. The S1 body consists of a top-most portion with wings-shaped bones on either end, known as the alae. The median ridge is a bony prominence located at the back of S1 vertebra. This ridge has bony openings (foramina), on both the right and left.
- L5 and the S1 facet joints are joined by articular cartilage lined lumbosacral joint.
- L5-S1 intervertebral disc. The disc between the vertebral bodies S5 and L5 is made of a gel-like material (nucleus pulposus). It is enclosed by a fibrous ring (annulus fibrosus). This disc acts as a shock absorber and cushion to protect the vertebrae when they move.
- L5 spinal cord. The L5 spinal neural roots exit the spinal cord through small bony foramina (intervertebral foramina) located on the left and the right sides of the spinal canal. These nerve roots are joined with other nerves and form larger nerves which travel down each leg.
- The L5 dermatome (or L5 skin area) receives sensations via the L5 spinal nerve and can include parts of the leg, foot and knee.
- The L5 myotome (a group of muscles controlled and coordinated by the L5 spine nerve) is responsible for leg and foot movement.
- The L5 – S1 motion segment provides a bony cover for the cauda equina (nerves running down from the spinal cord) and other delicate parts.
Common Problems in L5-S1
The L5 and S1 at the bottom, or vertebral column, are often under excessive biomechanical stress. This can cause more injuries and higher loads. The following are common problems:
- Disc problems. L5-S1 is the most common level for lower back disc herniation. An disc with a steeper angle will experience greater shear stresses. This can increase the disc’s risk of injury or degeneration.
- Facet joint pain. Facet joint discomfort can result from wear-and-tear arthritis (osteoarthritis), which is a result of the high load-bearing capacity of the lumbosacral joints.
- Spondylolysis. Spondylolysis can occur in the L5 vertebra. This is caused by repetitive stress on the bone. It can happen on one side or both. The bone may not break, but become stressed. This is called a “pars stress reaction”.
- Spondylolisthesis. Spondylolisthesis refers to a condition where the vertebrae slip over S1 if the L5 pars fracture on either side. Spondylolisthesis L5 occurs most often due to repetitive stress to L5’s pars interarticularis. This is most commonly seen in children or adolescents. Trauma is not a common cause of pars fracture.
- Although rare, malignant tumors like sacral chondromas can develop at the L5–S1 level. This level can also be affected by other problems, such as developmental variations in S1, the fusion of S5 and S1, or extra facet joints between S5-S1.
Common Symptoms and Signs of L5-S1 Stemming
L5-S1 vertebral and disc pain may develop gradually over time or suddenly after an injury. A dull ache, or sharp pain, may be felt in your lower back. Discogenic pain is often worsened when you sit too long, stand in one place, or do repetitive lifting and bending.
Radiculopathy symptoms, or sciatica may be caused by compression or inflammation of the L5/or S1 spinal neural nerve root.
- Pain is usually described as a sharp, shooting and/or severe sensation in the buttocks and/or toes.
- Numbness in the feet and/or toes
- Foot drop is a weakness in the foot or leg muscles.
- You can also experience a stabbing or aching sensation that is not related to these (dermatomal)areas. Although these symptoms are usually limited to one leg, they can also affect both legs at times.
Cauda Equina syndrome may develop at L5-S1 when there is an injury to the cauda Equina nerves, which descend from your spinal cord. This syndrome is a medical emergency. It typically causes severe pain, weakness or numbness and/or tingling in one or both legs. It is possible to lose bladder and/or bowel control. To preserve leg function and restore bladder and bowel function, the condition must be treated quickly.